Testosterone Levels by Age: The Complete Chart for Men What Your Numbers Actually Mean
If you have ever walked out of a lab with a testosterone result on paper and had absolutely no idea what it meant, you are not alone. Numbers like “412 ng/dL” are meaningless without context — specifically, context that accounts for your age.
That is the piece most articles miss. A testosterone level that is perfectly normal for a 55-year-old man could signal a serious hormonal issue in a 25-year-old. This guide gives you the full testosterone levels by age chart, explains what healthy testosterone range by age male looks like at every decade, and breaks down the real-world symptoms you should watch for as your levels naturally shift over time.
What Is Testosterone and Why Does It Change With Age?
Testosterone is the primary male sex hormone, produced mainly in the testes and, in small amounts, in the adrenal glands. It drives everything from muscle mass and bone density to libido, mood, and red blood cell production.
Here is the biological reality: testosterone does not stay constant throughout your life. It peaks during adolescence and early adulthood, then begins a slow, steady decline starting around age 30. According to research published in the Journal of Clinical Endocrinology & Metabolism, men lose roughly 1–2% of their total testosterone per year after age 30. That sounds minor, but compound that over two or three decades and the drop becomes clinically significant.
Understanding this decline and where your numbers fall on the age-adjusted spectrum — is the foundation of proactive men’s health.
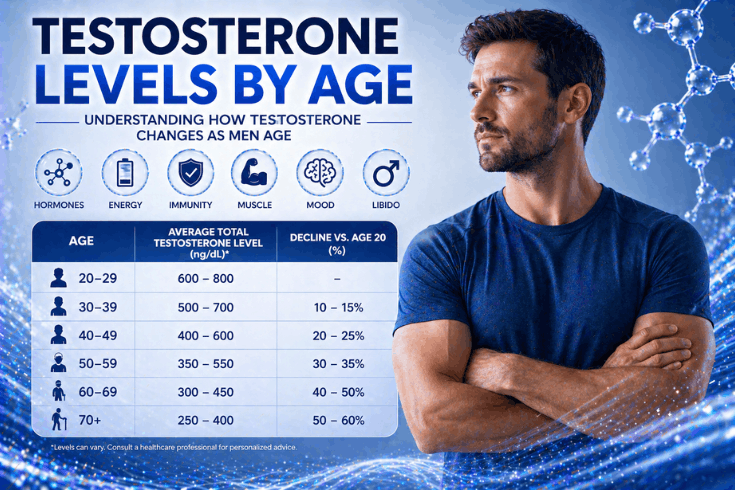
The ranges below represent total testosterone in nanograms per deciliter (ng/dL), the standard unit used by most labs in the United States. These are drawn from reference ranges published by major endocrinology bodies and clinical research studies.
| Age Range | Average Total Testosterone (ng/dL) | Decline vs. Age 20 (%) |
|---|---|---|
| 20–29 | 600 – 800 | — (peak levels) |
| 30–39 | 500 – 700 | 10 – 15% |
| 40–49 | 400 – 600 | 20 – 25% |
| 50–59 | 350 – 550 | 30 – 35% |
| 60–69 | 300 – 450 | 40 – 50% |
| 70+ | 250 – 400 | 50 – 60% |
Levels can vary based on individual health, lifestyle, and genetics. Consult a healthcare professional for personalized advice.
Important note: These ranges reflect total testosterone. Many clinicians also measure free testosterone the biologically active fraction not bound to proteins. Free testosterone gives a clearer picture of what your body can actually use, especially after age 50 when sex hormone-binding globulin (SHBG) tends to rise, lowering free testosterone even when total numbers appear adequate.
What Is a Healthy Testosterone Range by Age Male — Decade by Decade?
Teens (15–19): The Peak Is Building
Puberty triggers a dramatic testosterone surge. Levels can spike from near zero to well over 1,000 ng/dL in a matter of years. During this window, testosterone drives rapid muscle development, deepening of the voice, facial and body hair growth, and the development of reproductive organs.
Healthy range: 300–1,200 ng/dL depending on the exact age and stage of puberty.
What to watch: If a teenage boy shows delayed puberty signs (no growth of facial or pubic hair by 15–16, no testicular development), a testosterone test may be warranted to rule out hypogonadism.
20s (20–29): Peak Performance Window
This is the golden decade for testosterone. Most men hit their lifetime peak between ages 20 and 25. Energy is high, recovery is fast, muscle builds easily, and libido is strong.
Healthy range: 400–1,080 ng/dL | Optimal: 600–900 ng/dL
What to watch: A reading below 300 ng/dL in your 20s is a red flag and should prompt investigation into causes such as obesity, chronic stress, poor sleep, or a pituitary/testicular disorder — not assumed to be age-related.
30s (30–39): The Decline Begins — Quietly
This is where most men first notice subtle changes, even if their labs still appear “normal.” The decline is gradual roughly 1% per year but the cumulative effect of lifestyle factors (poor sleep, high cortisol from work stress, weight gain) can accelerate it.
Healthy range: 300–1,080 ng/dL | Optimal: 500–900 ng/dL
What to watch: If you notice a dip in gym performance, slower fat loss, or mild mood changes in your mid-to-late 30s, get your testosterone checked alongside a full hormone panel including LH, FSH, and prolactin.
40s (40–49): Clinically Meaningful Decline
The 40s are when testosterone decline becomes harder to ignore. The Endocrine Society defines late-onset hypogonadism low testosterone tied to aging as a total testosterone level below 300 ng/dL combined with clinical symptoms.
Healthy range: 252–916 ng/dL | Optimal: 400–800 ng/dL
What to watch: This is the decade where low testosterone symptoms by age start appearing with greater frequency. The most common include reduced libido, increased body fat (especially around the abdomen), difficulty maintaining muscle mass, and lower energy. These overlap with many other conditions, so lab confirmation is essential before attributing symptoms to testosterone alone.
50s (50–59): Free Testosterone Matters More
By your 50s, SHBG levels are typically rising, binding more testosterone and reducing the free fraction. A man in his 50s may have a “normal” total testosterone of 500 ng/dL but a low free testosterone, which explains symptoms despite seemingly adequate total levels.
Healthy range: 215–878 ng/dL | Optimal: 350–700 ng/dL
What to watch: Request both total and free testosterone panels. Also consider checking estradiol (E2), as aromatase activity (which converts testosterone to estrogen) tends to increase with body fat accumulation.
60s and Beyond (60+): Managing the New Normal
Testosterone continues declining, and by age 70, many men have levels around 300–400 ng/dL or lower. This is clinically classified as age-related hypogonadism when accompanied by symptoms, but whether treatment is appropriate depends on individual health goals, cardiovascular risk, and physician evaluation.
Healthy range (60–69): 196–859 ng/dL | Optimal: 300–650 ng/dL Healthy range (70+): 156–700 ng/dL | Optimal: 250–600 ng/dL
What to watch: At this stage, bone density, mood, cognitive clarity, and cardiovascular health all intersect with testosterone levels. Discuss annual hormone panels with your physician as a standard part of men’s preventive care.
Low Testosterone Symptoms by Age: What to Actually Look For
Symptoms of low testosterone are not always dramatic. They tend to creep in gradually, and because they mimic general aging or lifestyle-related complaints, many men dismiss them for years. Here is how low testosterone symptoms by age tend to present:
In Your 20s and 30s:
- Persistent fatigue despite adequate sleep
- Reduced sex drive or difficulty achieving erections
- Difficulty building or maintaining muscle despite consistent training
- Low mood, irritability, or mild depression
- Brain fog or difficulty concentrating
- Decreased motivation or competitive drive
In Your 40s:
- All of the above, often more pronounced
- Noticeable increase in body fat, particularly visceral (belly) fat
- Reduced bone density or frequent minor injuries
- Thinning body or facial hair
- Night sweats or sleep disturbances
- Declining strength despite maintaining workout routines
In Your 50s and Beyond:
- Significant reduction in libido
- Erectile dysfunction (in combination with other hormonal or vascular factors)
- Increased risk of osteoporosis or fractures
- Cognitive changes, including difficulty with memory or mental sharpness
- Cardiovascular risk markers shifting unfavorably
- Depression or significant loss of motivation
Critical distinction: None of these symptoms alone confirm low testosterone. Many overlap with thyroid dysfunction, sleep apnea, insulin resistance, and depression. Always pair symptom review with laboratory testing before drawing conclusions.
How Is Testosterone Actually Tested?
Understanding a testosterone levels by age chart is only useful if you are testing correctly. Here are the key variables:
Timing matters: Testosterone follows a circadian rhythm, peaking in the early morning. Labs should be drawn between 7:00 AM and 10:00 AM for the most accurate reading. Testing in the afternoon can yield results 15–25% lower than your true baseline.
What to test:
- Total Testosterone
- Free Testosterone (or calculated free T using SHBG and albumin)
- SHBG (Sex Hormone-Binding Globulin)
- LH (Luteinizing Hormone) — helps determine if the issue is in the testes or the pituitary
- FSH (Follicle-Stimulating Hormone)
- Estradiol (E2)
- Prolactin (to rule out pituitary adenoma)
One reading is not enough: A single low result is not sufficient for a clinical diagnosis. The Endocrine Society recommends at least two morning measurements on separate days before confirming hypogonadism.
What Can Lower Testosterone at Any Age?
Even if you are in your optimal age window, several modifiable factors can tank your testosterone:
- Obesity and excess body fat: Adipose tissue converts testosterone to estrogen via aromatase. More fat generally means lower testosterone.
- Chronic sleep deprivation: Studies show that sleeping fewer than 5 hours per night can reduce testosterone by 10–15% in just one week.
- Chronic psychological stress: Elevated cortisol directly suppresses testosterone production at the hypothalamic-pituitary level.
- Alcohol overconsumption: Regular heavy drinking impairs Leydig cell function in the testes.
- Sedentary lifestyle: Resistance training is one of the most consistent natural testosterone boosters. Inactivity trends in the opposite direction.
- Poor diet: Extremely low-fat diets can suppress testosterone since cholesterol is a direct precursor to its synthesis.
- Certain medications: Opioids, corticosteroids, and some antidepressants are known to suppress testosterone production.
The good news: many of these factors are reversible. Lifestyle optimization before considering pharmacological intervention is always the first step.
Should You Consider Testosterone Replacement Therapy (TRT)?
Testosterone Replacement Therapy is one of the most discussed and most misunderstood interventions in men’s health today. Before considering it, it is critical to understand what TRT is actually designed for and what the treatment process genuinely involves.
TRT is a medical treatment, not a performance enhancement strategy. It is clinically validated specifically for men diagnosed with hypogonadism — a condition where the body does not produce sufficient testosterone to meet physiological needs. It is not appropriate for men whose levels fall within the normal range for their age, even if those men feel “not quite right.” Chasing peak numbers without clinical indication creates more risks than benefits.
The diagnosis must be airtight. Before a physician prescribes TRT, the process should follow a clear clinical protocol:
- Two confirmed low readings: A single low testosterone result is not enough. Testing must be repeated on two separate mornings — between 7:00 AM and 10:00 AM — since testosterone peaks in the early hours and a single afternoon draw can produce a falsely low result.
- Presence of clinical symptoms: Lab numbers alone do not justify treatment. The patient must also present with symptoms consistent with hypogonadism — such as persistent fatigue, reduced libido, loss of muscle mass, mood disturbances, or erectile dysfunction — linking the biochemical finding to real functional impact.
- Reversible causes must be ruled out first: Obesity, obstructive sleep apnea, chronic psychological stress, opioid use, and certain antidepressants are all documented causes of secondary low testosterone. Addressing these factors first can restore levels without pharmacological intervention.
- Full health evaluation: Because TRT affects multiple body systems, physicians must assess cardiovascular health, baseline PSA levels (prostate-specific antigen), hematocrit (red blood cell concentration), and the patient’s fertility goals before initiating therapy.
- Ongoing monitoring is non-negotiable: Once on TRT, regular blood work every 3–6 months is required to track hematocrit (TRT can thicken the blood, raising clot risk), PSA (to screen for prostate changes), estradiol levels (excess testosterone converts to estrogen), and overall symptom response.
Fertility is a critical consideration. TRT suppresses the body’s own testosterone production by signaling the brain to stop releasing LH and FSH — the hormones that also drive sperm production. Men who want to father children should not start TRT. Instead, medications such as clomiphene citrate (a selective estrogen receptor modulator that stimulates natural testosterone production) or human chorionic gonadotropin (HCG) (which mimics LH and supports both testosterone and sperm production) are the preferred alternatives in fertility-preserving protocols.
The bottom line: TRT, when properly indicated and carefully managed, can meaningfully improve quality of life. When used without proper evaluation, it carries real risks cardiovascular strain, infertility, polycythemia, and hormonal imbalance. The process matters as much as the treatment itself.
Conclusion
Testosterone is not just a number on a lab report — it is one of the most telling biomarkers of a man’s overall health at every stage of life. Understanding where your levels stand on the testosterone levels by age chart gives you something far more valuable than raw data: it gives you context.
From the peak years of your 20s through the gradual decline of your 50s and beyond, what matters most is whether your levels are appropriate for your age, aligned with how you feel, and supported by a lifestyle that gives your body every opportunity to thrive naturally.
The chart matters. The symptoms matter. The testing protocol matters. Before reaching for pharmaceutical solutions, prioritize the fundamentals — quality sleep, resistance training, healthy body composition, and stress management. These alone can meaningfully shift the needle for most men.
Know the healthy testosterone range by age male, recognize low testosterone symptoms by age before they compound, and always work with a physician who treats the full clinical picture not just a single result.
Your hormonal health is not fixed. With the right knowledge and the right habits, it is something you can actively protect at every decade.
Frequently Asked Questions
What is a dangerously low testosterone level?
Most clinicians consider total testosterone below 200–250 ng/dL as clinically low regardless of age and warranting evaluation and likely treatment.
Can you have low testosterone but still feel fine?
Yes. Individual androgen receptor sensitivity varies significantly. Some men function well at 280 ng/dL; others feel significant symptoms at 350 ng/dL. This is why symptoms must be evaluated alongside laboratory values.
Does testosterone affect heart health?
The relationship is complex. Severely low testosterone is associated with increased cardiovascular risk. However, the cardiovascular safety of TRT has been a subject of ongoing research. The FDA-approved TRAVERSE trial (2023) provided reassurance that TRT in men with hypogonadism and moderate cardiovascular risk does not significantly increase major adverse cardiovascular events.
How often should men check their testosterone?
Annual testing is reasonable starting at age 35–40, or earlier if symptoms are present. Men on TRT typically require testing every 3–6 months.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before making decisions about hormone testing or treatment.
