How Testosterone Replacement Therapy Actually Works Inside Your Body The Biology, Step by Step
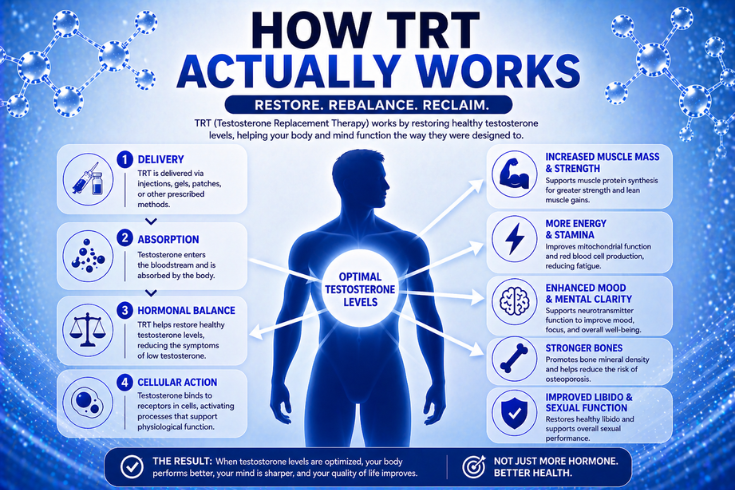
What Is TRT, and Why Does It Matter?
If you’ve been feeling persistently fatigued, noticed a dip in your motivation, or found that your body just doesn’t respond to exercise the way it used to you’re not alone. Millions of men around the world quietly experience the effects of low testosterone, often without knowing that a medically recognised solution exists.
TRT explained simply: Testosterone Replacement Therapy (TRT) is a medically supervised treatment that restores testosterone to healthy levels in men whose bodies no longer produce enough on their own. But what actually happens inside your body when you begin? How does an injection, gel, or patch translate into feeling more like yourself again?
To get TRT explained properly, you need to look beyond the label and understand the real biology. This guide breaks it down step by step, cell by cell — so you know exactly what’s happening beneath the surface. Whether you’ve just received a diagnosis or you’re exploring your options, this is the clearest, most complete picture of how hormone replacement therapy works in real human biology.
Understanding Testosterone: The Hormone Behind the Scenes
Testosterone is often reduced to a symbol of masculinity, but its real role is far more complex and essential. It is a steroid hormone produced primarily in the testes and in smaller quantities in the adrenal glands. Women also produce testosterone, though in much lower amounts.
What Does Testosterone Actually Do?
Testosterone doesn’t just affect one system it influences your entire body:
- Muscles and bones: Stimulates protein synthesis, building lean muscle mass and maintaining bone density
- Brain and mood: Influences dopamine pathways, contributing to motivation, confidence, and emotional stability
- Energy metabolism: Regulates how efficiently your body converts food into usable energy
- Sexual function: Drives libido and supports erectile function
- Red blood cell production: Signals bone marrow to produce more red blood cells, improving oxygen delivery
- Fat distribution: Helps regulate where and how the body stores fat
The HPG Axis: Your Body’s Internal Thermostat
Testosterone production is governed by a feedback loop called the Hypothalamic-Pituitary-Gonadal (HPG) Axis:
- The hypothalamus releases Gonadotropin-Releasing Hormone (GnRH)
- GnRH signals the pituitary gland to release Luteinising Hormone (LH) and Follicle-Stimulating Hormone (FSH)
- LH travels to the testes, triggering testosterone production in Leydig cells
- When levels rise, the hypothalamus slows GnRH — a natural feedback brake
When this system malfunctions due to age, injury, illness, or other factors, testosterone production falls. That’s where low testosterone treatment, including TRT, becomes medically relevant.
What Happens When Testosterone Drops?
Low testosterone clinically called hypogonadism doesn’t always announce itself with obvious symptoms. It tends to arrive quietly, disguised as everyday complaints.
Common Signs of Low Testosterone
| Symptom Category | What You May Notice |
|---|---|
| Physical | Fatigue, reduced muscle mass, increased body fat, hair thinning |
| Sexual | Low libido, erectile difficulties, reduced ejaculate volume |
| Psychological | Brain fog, low mood, irritability, reduced drive |
| Metabolic | Weight gain, poor blood sugar regulation, sluggish recovery |
Quick Answer: If you experience three or more of these symptoms consistently, a simple blood test can confirm whether your testosterone falls below the clinical threshold generally below 300 ng/dL in most guidelines.
Why Does Testosterone Decline in the First Place?
Testosterone levels naturally begin declining after age 30 — typically by around 1% per year. But age isn’t the only cause:
- Primary hypogonadism: The testes themselves fail to produce adequate testosterone due to injury, infection, or conditions like Klinefelter syndrome
- Secondary hypogonadism: The hypothalamus or pituitary gland fails to send the right signals — caused by obesity, chronic stress, sleep deprivation, or pituitary disorders
- Lifestyle factors: Chronic alcohol use, poor sleep, extreme caloric restriction, and prolonged stress can suppress testosterone production over time
Understanding the root cause of low testosterone shapes which form of low testosterone treatment — including whether TRT is appropriate is right for each individual.
TRT Explained: How It Works Step by Step
Here’s where the biology gets genuinely fascinating. When you introduce exogenous (externally supplied) testosterone into your body, a precise biological cascade unfolds. Having TRT explained at this cellular level is key to understanding why results take time and why regular monitoring matters so much.
Step 1: Testosterone Enters the Bloodstream
Regardless of delivery method injection, gel, patch, or pellet testosterone is absorbed into the bloodstream. From here, it travels bound to proteins, primarily Sex Hormone-Binding Globulin (SHBG) and albumin.
Only free testosterone (the unbound fraction, typically 1–3%) is biologically active and able to enter cells.
Step 2: Testosterone Binds to Androgen Receptors
Once free testosterone reaches a target cell in muscle, bone, brain, or skin it crosses the cell membrane and binds to an androgen receptor (AR) inside the cell.
Think of this as a key fitting into a lock. When testosterone (the key) meets the androgen receptor (the lock), it activates the entire mechanism.
Step 3: Gene Expression Changes
The activated testosterone-receptor complex travels into the cell nucleus and binds to specific DNA regions called androgen response elements (AREs). This triggers or suppresses the expression of particular genes.
In muscle cells, this means increased production of proteins needed for growth and repair. In the brain, it influences neurotransmitter activity including dopamine and serotonin pathways — which is why mood and motivation often improve with well-managed therapy.
Step 4: Conversion Testosterone Becomes Other Hormones
Not all testosterone remains as testosterone. Some undergoes conversion:
- Estradiol (oestrogen): Via the enzyme aromatase, testosterone is partially converted to oestrogen — necessary for bone health, cardiovascular function, and libido in men
- Dihydrotestosterone (DHT): Via the enzyme 5-alpha reductase, testosterone converts to DHT — a more potent androgen that affects hair follicles and the prostate
This is why good TRT management involves monitoring not just testosterone, but also oestrogen and DHT levels.
Step 5: The Feedback Loop Responds
As exogenous testosterone raises blood levels, the HPG axis signals its own slowdown. The hypothalamus cuts back on GnRH, the pituitary reduces LH and FSH, and the testes slow or pause their natural output.
This is expected and well-managed within responsible hormone replacement therapy protocols.
How Different TRT Delivery Methods Work in the Body
Not all testosterone is delivered the same way — and each method creates a different absorption and stability profile. Understanding the options is part of getting TRT explained in a way that’s clinically useful before you and your doctor make a decision.
Intramuscular Injections (e.g., Testosterone Cypionate, Enanthate)
Injected into muscle tissue, usually every 1–2 weeks. Levels peak within 24–72 hours and gradually decline. Some men notice noticeable energy shifts as levels fluctuate between doses.
Transdermal Gels and Creams
Applied daily to the skin, gels allow testosterone to absorb steadily — mimicking more natural daily rhythms. Levels are more stable than with injections, but there is a small risk of skin-to-skin transfer to others.
Testosterone Patches
Similar to gels, patches deliver a consistent daily dose through the skin. They’re discreet but can occasionally cause mild irritation at the application site.
Subcutaneous Pellets
Small pellets inserted under the skin — typically near the hip — release testosterone slowly over 3–6 months. This offers one of the most stable, low-maintenance options available.
Oral and Buccal Formulations
Newer oral formulations (like testosterone undecanoate) and buccal tablets are available, though less commonly prescribed. They bypass some — but not all — liver metabolism concerns.
TRT Benefits: What Changes Inside You
When testosterone levels are restored to a healthy physiological range, the effects can be meaningful — but they unfold gradually, not overnight. This is one of the most important things to understand when getting TRT explained by a healthcare professional.
A Realistic Timeline of TRT Benefits
| Timeframe | What You May Notice |
|---|---|
| Weeks 1–2 | Improved sleep quality, subtle mood lift |
| Weeks 3–6 | Increased energy, early libido improvements, reduced brain fog |
| Weeks 6–12 | Noticeable gains in strength, improved body composition begins |
| Months 3–6 | Sustained muscle development, fat reduction, sexual health improvements |
| 6–12 months | Bone density improvements, stabilised hormone levels, full benefit realisation |
Physical Changes (Weeks 3–12+)
- Increased lean muscle mass when combined with resistance training
- Reduction in stubborn body fat, particularly visceral fat
- Improved bone mineral density over time
- Better exercise recovery and endurance
Cognitive and Emotional Shifts (Weeks 2–6)
- Improved mental clarity and focus
- Reduction in low mood and irritability linked to hypogonadism
- Greater motivation and sense of purpose
Sexual Health Improvements (Weeks 3–6)
- Increased libido and sexual interest
- Improvements in erectile function, especially when combined with appropriate care
- Greater overall sexual satisfaction
Important: TRT benefits are most pronounced in men with clinically confirmed low testosterone — not in those whose levels are already in the normal range. Individual results vary significantly.
TRT Side Effects and Safety Considerations
TRT safety deserves honest, balanced discussion. Like any medical treatment, testosterone therapy carries potential risks that must be carefully weighed against benefits — and this is part of why TRT explained in a clinical setting always includes a thorough risk assessment.
Common Side Effects
- Erythrocytosis: TRT stimulates red blood cell production, which can increase blood viscosity — regular haematocrit monitoring is essential
- Acne and oily skin: Elevated androgen activity can increase sebum production
- Fluid retention: Some men experience mild water retention, particularly early in treatment
- Mood fluctuations: Often related to suboptimal dosing or level peaks and troughs between doses
Serious Considerations
- Cardiovascular health: The evidence is nuanced. Responsible prescribing involves cardiovascular screening and ongoing monitoring
- Prostate health: TRT is contraindicated in men with untreated prostate cancer; regular PSA monitoring is standard practice
- Sleep apnoea: TRT may worsen pre-existing sleep apnoea in some individuals
Who Should Avoid TRT?
TRT is generally not recommended for men with:
- Untreated prostate or breast cancer
- Severe, uncontrolled cardiovascular disease
- A desire to preserve natural fertility without adjunct therapy
- High haematocrit levels at baseline
TRT and Fertility: What You Should Know
One of the most commonly misunderstood aspects of testosterone replacement therapy is its impact on fertility. Because exogenous testosterone suppresses the HPG axis — reducing LH and FSH — sperm production (spermatogenesis) decreases significantly during treatment. This is an important part of TRT explained honestly to any man considering therapy.
This does not mean permanent infertility. For men wishing to father children, alternative protocols can be used alongside or instead of TRT to maintain sperm production.
Options for Men Who Want to Preserve Fertility
- HCG (Human Chorionic Gonadotropin): Mimics LH, directly stimulating the testes to continue producing testosterone and sperm — can be used alongside TRT
- Clomiphene citrate (Clomid): An oral medication that blocks oestrogen receptors in the hypothalamus, stimulating the body’s own LH and FSH production naturally
- Sperm banking: Some men choose to bank sperm before beginning TRT as a precautionary step
This is why an open, detailed conversation with a specialist before starting any low testosterone treatment is absolutely essential.
Myths vs. Facts: A Quick Comparison Table
| Myth | Fact |
|---|---|
| TRT is just for bodybuilders | TRT is a medical treatment for clinically diagnosed hypogonadism |
| TRT causes prostate cancer | Current evidence does not support this; prostate health is carefully monitored |
| You’ll feel results in days | Benefits typically emerge over weeks to months of consistent treatment |
| TRT permanently shuts down natural production | Natural production often resumes after stopping, particularly with proper protocols |
| TRT is dangerous for the heart | Risk is nuanced and patient-specific; responsible prescribing minimises cardiovascular risk |
| Once you start, you’re on it forever | Duration depends on diagnosis, goals, and individual response — it is not always lifelong |
Conclusion:
TRT explained at its core is this: a medically supervised process of restoring a hormone your body depends on for energy, strength, mood, and long-term health — when it can no longer produce enough on its own.
The biology is elegant. Testosterone enters your system, binds to receptors at a cellular level, changes gene expression, and triggers a meaningful cascade of physical and psychological improvements. It is not magic — it is physiology, carefully guided by clinical oversight.
Understanding how testosterone replacement therapy works — from the HPG axis to androgen receptor binding, from hormone conversion to feedback suppression — gives you the foundation to have a more informed conversation with your doctor and set realistic expectations. TRT is not a quick fix. It is a gradual, consistent process of hormonal restoration that rewards patience and commitment.
What TRT is not is a shortcut, a cure-all, or a decision to take lightly. It works best when personalised, properly monitored, and supported by healthy daily habits — including quality sleep, balanced nutrition, regular exercise, and stress management.
If you are experiencing symptoms of low testosterone — fatigue, low mood, reduced strength, or diminished libido — the first step is always a conversation with a qualified healthcare professional. A blood test and an honest clinical assessment will guide you far better than any article alone.
Your hormones are a lifelong system. Treat them with the care they deserv
Frequently Asked Questions
How long does it take for TRT to work?
Most men begin noticing improvements in energy and mood within 3–6 weeks. Muscle and sexual health changes typically take 3–6 months of consistent therapy to fully emerge.
Is TRT safe long-term?
When properly managed with regular blood monitoring, TRT has been used safely in clinical settings for decades. Ongoing research continues to refine best practices around long-term TRT safety.
Will TRT make me infertile?
TRT suppresses sperm production during use, but this is generally reversible. Men concerned about TRT and fertility should discuss adjunct therapies with their doctor before beginning treatment.
Can I stop TRT once I start?
Yes, but it should be done under medical supervision. Stopping abruptly can cause a temporary decline in testosterone as the body’s natural production resumes. A tapering protocol is often recommended.
How is testosterone deficiency diagnosed?
Diagnosis requires a blood test measuring total testosterone — ideally taken in the morning when levels peak — alongside a full symptom assessment. A second confirmatory test is usually required before any low testosterone treatment begins.
Does TRT cause mood swings?
Poor dosing or fluctuating hormone levels can trigger mood changes. A well-managed protocol with stable, consistent levels typically reduces — rather than causes — mood instability.
What blood tests are needed during TRT monitoring?
Regular monitoring typically includes total and free testosterone, haematocrit, PSA, oestradiol, LH, FSH, and a full metabolic panel. Your doctor adjusts testing frequency based on how stable your levels remain over time.
Is there a natural way to boost testosterone before trying TRT?
For mild cases, lifestyle changes resistance training, better sleep, reduced alcohol, weight management, and stress reduction — can meaningfully support testosterone levels. However, for clinically confirmed hypogonadism, lifestyle changes alone are rarely sufficient to restore optimal levels, and TRT or an equivalent low testosterone treatment may be necessary.
DESCLAIMER: This article is for educational purposes only. It does not constitute medical advice, diagnosis, or treatment. Consult a licensed medical professional before making any decisions about hormone therapy.
